Reshaping Health Care

Building on long-standing strengths in data analytics, biology and other fields, Lehigh has identified two areas of focus for its proposed College of Health—Innovation in Value-Based Health Care, and Biological and Social Determinants of Health—as it takes significant steps toward a 2020 opening.
Lehigh also has begun a search for the college’s inaugural dean, and this fall will begin recruiting the first group of faculty for a Fall 2019 start.
The college’s focus areas are “still relatively broad so those who get involved will have an opportunity to further define, clarify, probably further focus these themes,” said Provost Pat Farrell at a Town Hall on campus in late March. But they’re clear enough, he said, for the Lehigh community to see where the University can really make an impact in health care.
As defined, Innovation in Value-Based Health Care would allow faculty to examine the quality and effectiveness of care that’s provided to individuals and populations, with the aim of providing better outcomes for patients. The work could have an impact on global and domestic policy as industry leaders and providers work to improve health care delivery.
Faculty working in the area of Biological and Social Determinants of Health would strive to better understand the major drivers of health and seek the root causes of health disparities among populations. Areas to be explored would include genetics, environmental factors, family and community health and health economics.
At its core, the College will be interdisciplinary.
“We’d like to have a College that has very low walls around it, so those who are inside easily can go outside—faculty, staff and students—to do their work, to collaborate, to find other people to work with,” Farrell said, “and those who are outside find their way in easily as well.” He pointed to course work, faculty collaborations and staff partnerships. Though collaborations happen now on campus, he said, “We have a chance to design a College where we might really intentionally make that almost always true, and I think we want to take that opportunity.”
Planning continues with input from internal and external stakeholders.
“I’m expecting that the academic result—meaning new courses, new learning, new research—begins the day faculty show up on campus,” Farrell said.
Lehigh initially worked with Boston Consulting Group to better understand the health care landscape and determine where the new College should focus its attention and effort. Since December 2017, its work with Strategy+ has focused on the College’s operational framework. The consulting group is preparing a report with recommendations for next steps.
Farrell said he and Lehigh President John D. Simon met with about 20 health care networks to discuss the plans for the College. Network representatives are excited about the talent the new College will produce and the collaborative research opportunities it will provide, he said.
“I think our opportunity space here is really to produce a graduate with a somewhat different skill set from traditional clinical health graduates or health graduates that come from other kinds of more traditional health organizations,” said Farrell. “That’s our big advantage, and I’d like us to think about how do we do that in a distinct and innovative way.”
The College of Health is a key component of Lehigh’s Path to Prominence, an ambitious plan outlined by Simon that would add 1,000 undergraduates, 500 graduate students and 100 new faculty members. The initiative will allow Lehigh to build on its legacy, broaden its academic footprint and foster an ever more vibrant atmosphere of creativity and collaboration.
Faculty research in the health arena has been ongoing across a variety of disciplines. Researchers are tackling a host of problems that include Ebola, opioid addiction and cancer, among many others. Here is some of the research under way.
A Better Understanding of Ebola
A mother brings her sick child for treatment in Liberia during the 2015 Ebola outbreak.
In 2014-2015, the Ebola virus spread across West Africa and killed more than 10,000 people.
“So far, there is no cure,” says Frank Zhang, associate professor of bioengineering and mechanical engineering and mechanics.
Just how the Ebola virus infects its host cell isn’t entirely clear. Zhang and Anand Jagota, founding chair of the Department of Bioengineering, believe that quantitative knowledge about how Ebola interacts with the T-cell immunoglobulin and mucin (TIM) family of proteins can help them predict the conditions for Ebola’s attachment to the host cell.
Compared to HIV or influenza, Ebola is a large virus—about one-tenth the size of a human cell. To enter a human cell, Ebola takes advantage of a natural process called macropinocytosis, through which the cell “cleans up” its surroundings by internalizing and eventually destroying the dead cell debris that surrounds it. T-cell immunoglobulin and mucin domain (TIM) proteins serve as cell-surface receptors and allow immune cells to recognize the dead cell debris and internalize it. Ebola interacts with the TIM proteins and uses them to hijack this important physiological process, which essentially welcomes the virus into the cell.
Once inside the cell, the virus membrane fuses to the endosome that has formed around it and releases its genetic content into the cell like the proverbial Trojan Horse.
“Viral RNA further hijacks the cell mechanism to make proteins,” says Zhang. “At that stage these replicate themselves inside and then they bud off the membrane to form the new virus. Along this process, of course, our cells die and that generates the problem.”
Rather than a vaccine, which may not always be effective, says Zhang, one approach might be a drug that would inhibit Ebola’s ability to replicate. This approach has two possible strategies: The first involves blocking the step in which the virus enters the human cell. The second involves blocking the step in which the viral membrane fuses to the endosomal membrane. Researchers are currently testing drugs that take the second approach, says Zhang, “but, of course, this is not as good as if you can prevent the virus from entering the cell in the first place.”
Zhang and Jagota seek to understand how the Ebola virus interacts with the cell membrane and gets internalized so they can eventually help to design a drug that will prevent Ebola from entering the cell while still allowing the natural internalization process of dead cells to take place. First they must determine the differences between Ebola and cell debris.
Zhang uses an atomic force microscope (AFM), which scans the surface of a very small sample to determine its mechanical properties: its shape, softness or stiffness. He uses a virus-like particle (VLP), which has the same shape and shell as the Ebola virus but not its genetic materials.
“[We discovered that] the shape and the mechanical properties of cells and VLP are very different,” says Zhang. “Cells are usually pretty soft [and, in many cases, round], especially when they die, and Ebola is thin and long and very stiff. … We thought maybe we can utilize this difference, and we can hopefully design a drug that would block this stiffer object from coming into the cell but not block the natural process where the cell ingests a soft and round object.”
In another experiment using the AFM, Zhang brings the VLP to the cell with its TIM receptor expressed, observes their interaction, and pulls them apart to determine the mechanical strength of the interaction, or how much force is required to pull them apart.
Jagota uses mathematical models to understand the interaction between Ebola and the cell, what properties represent the Ebola virus—its stiffness, its shape—and what properties represent the cell—the components it presents on its surface—in this interaction.
Zhang and Jagota’s project is supported by the National Institutes of Health (NIH). A grant from the National Science Foundation (NSF) will support parts of the modeling phase of their work.
Examining the Health Implications of Fracking
A chest X-ray of pneumonia in a 72-year-old woman.
Unconventional natural gas development of Marcellus shale in Pennsylvania, also known as “fracking,” has become more common in recent years—as has concern over how the practice might impact the health of those living near extraction sites.
Former Lehigh doctoral student Lizhong Peng, Chad Meyerhoefer, professor of economics, and Shin-Yi Chou, professor and chair of economics, wanted to know the extent to which fracking increases hospitalizations for air-pollution sensitive conditions. Their paper, “The health implications of unconventional natural gas development in Pennsylvania,” was published earlier this year in the journal Health Economics.
“Despite the fact that air pollution has clear adverse health effects, there is little scientific research on the impact of shale gas development on human health,” the team writes. They cite a 2015 paper that examined two Pennsylvania counties between 2007 and 2011 and reported that shale gas development during that time is significantly associated with increased hospitalization for cardiology and neurology patients, among others. The Lehigh team built upon this study by including all of Pennsylvania and by extending the time frame from 2001 to 2013.
The team merged well permit data from the Pennsylvania Department of Environmental Protection with a database of all inpatient hospital admissions from 2001 to 2013 to compare changes in hospitalization rates over time for air pollution–sensitive diseases in counties with unconventional gas wells to changes in hospitalization rates in counties without wells.
“We aggregated these data up to the county level, merged them and started to look for patterns in disease rates that correspond to high-fracking and low-fracking areas. It took a long time for us to actually tease out the effects because it’s a really difficult problem to look at,” says Meyerhoefer.
The researchers controlled for changes in the amount of natural gas output, coal production and county-level demographics. They also used synthetic control methods to track the change in hospitalization rates over an extended period of time in counties with and without fracking.
Bradford County, for example, has high levels of fracking. The team examined other Pennsylvania counties that did not have fracking but had comparable characteristics to Bradford County. Like taking a weighted average, says Meyerhoefer, they used these similar counties to create a control unit—a synthetic county—that looks like Bradford, but that does not have fracking. The team then looked at the change in disease rates in Bradford relative to the synthetic county they’d created.
“Our findings provide evidence of adverse health effects of unconventional natural gas development,” says Meyerhoefer.
Specifically, the team found that fracking increased rates of hospitalization for pneumonia among elderly Pennsylvania residents by 6 to 9 percent. This, the researchers report, is consistent with the higher levels of air pollution that result from unconventional natural gas development. The negative health effects of fracking were concentrated among the elderly rather than among children.
“This is surprising because children spend a greater portion of their day outdoors,” says Meyerhoefer. “This could be because the negative health effects of fracking experienced by children did not result in hospitalization or because there were changes in child migration that were not fully controlled for in our models.”
The study’s results could potentially help policymakers determine the most effective method of taxation for fracking. The team’s findings, based on the timing of when health effects occur, suggest that “it’s actually not so much the extraction of the gas that causes the pollution—it’s the development of the well site,” says Meyerhoefer. “As a result, there is more justification for well-permitting fees than gas extraction taxes as a means to account for the negative externalities associated with fracking.”
In Pursuit of the Deadly Tumor Cell
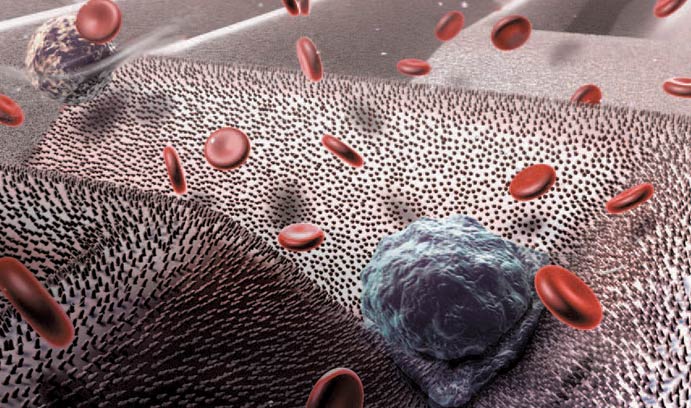
The biomimetic features on the capture pad of Liu's chip are designed to adhere to tumor cells while allowing normal blood cells to flow past.
For years, bioengineer Yaling Liu has been in pursuit of the deadly tumor cell. Liu has been perfecting a microfluidic device the size of two quarters that has the ability to catch and release circulating tumor cells (CTCs)—cancer cells that circulate in a cancer patient’s blood. Such a device could lead to earlier detection of primary tumors and metastasis, as well as determine the effectiveness of treatment—all through a simple, non-invasive blood test.
Liu, professor of mechanical and bioengineering, is in the early stages of testing his device in a clinical setting—and the results are promising.
Liu’s “lab on a chip” is notable for its ability to not only capture circulating tumor cells, but to “release” those cells as well.
“Our circulating tumor cell device can release a tumor cell captured from a blood sample, enabling single cell analysis,” says Liu. “It could be used to check the effectiveness of treatment, by identifying the amount of tumor cells circulating. Conducting genetic testing on a released single cell could also reveal whether the primary tumor had metastasized, as metastasized cells have unique genetic markers.”
The device, which could also be used to check the effectiveness of cancer gene therapy, is part of a clinical drug trial for melanoma and renal cancers at the Lehigh Valley Cancer Institute. Funding for the study has been provided by the Andy Derr Foundation for Kidney Cancer Research. The goal is to gather preliminary data about whether the device can improve care.
The first stage of the trial, which involved an analysis of circulating tumor cells from a single blood draw of several dozen patients, has demonstrated strong potential.
“The next step will be to track a few patients over the course of their treatment, taking several blood draws to see if the data captured by the microfluidic device correlates with the data their medical team is collecting through other methods,” says Liu.
Liu’s microfluidic device achieves two key standards by which the success of CTC devices is measured: high capture efficiency and high selectivity. Capture efficiency refers to the percentage of CTCs that the device collects. Selectivity measures how well it rejects unwanted cells, such as red and white blood cells.
The rectangular chip—smaller than a few square centimeters and using as little as a few milliliters of blood—is made of the polymer PDMS. The chip’s key feature is a tiny flow channel on a hierarchically designed pad that is optimized to capture tumor cells from the blood flowing across it.
Using microfluidic design principles, Liu’s group engineered vortices in their device to increase the chance that tumor cells will collide with the surface of the flow channel. The group also arranged ripples in a wavy-herringbone pattern lining the bottom of the capture pad.
“The herringbone surface generates a passive vortex that mixes the cells and increases the chance that they will collide with the capture pad,” says Liu. “High selectivity is achieved by smoothing the sharp grooved herringbone pattern into a wavy one, helping to filter out unwanted cells.”
The group uses immunoaffinity—the specific chemical affinity between an antibody and an antigen—to make CTCs adhere to the device while normal blood cells flow past. They coat the pad with a layer of anti-epithelial cell adhesion molecules (anti-EpCAM) which bond with CTCs but not with normal cells.
“With metastatic cancers accounting for around 90 percent of deaths from solid tumors,” says Liu, “the hope is that one day a device that can enable the analysis of single tumor cells circulating in the blood could make a big difference in early diagnosis, detection and monitoring of numerous types of cancer, without invasive biopsies.”
Addressing Community Health Issues

Faculty members who form Lehigh’s Community Health Research Group are forging relationships with community members, nonprofit organizations and health care providers in the Lehigh Valley in an effort to understand and address health needs and health disparities in the region. In one project, researchers are partnering with a health organization to evaluate the effectiveness of an innovative opioid addiction treatment program, and in another, exploring social integration and well-being among racially and economically marginalized populations.
Led by Christopher Burke, associate professor of psychology, the interdisciplinary faculty group includes Sirry Alang, assistant professor of sociology and anthropology and Health, Medicine and Society; Kelly Austin, associate professor of sociology; Julia Lechuga, assistant professor of education and Health, Medicine and Society; and Lucy Napper, assistant professor of psychology. It aims for a Community-Based Participatory Research approach, which values collaboration with community members throughout the research process.
“Everybody has some expertise that they bring to the project,” says Burke. “While the academic partners might have methodological expertise and content expertise from their research literatures, the community members and organizational partners have the expertise of their lived experiences. They know about the neighborhood, they know about the people, they know how things work, they know how to get things done, they know who to talk to.”
There are conversations about interests, skills and strengths, Burke says. “That’s also a way of trying to demonstrate that the community does have something to give, that it’s not just a place where there are problems that researchers can come down and try to solve,” he said. “It’s a place where there’s a lot of life and activity. The question is, could working together with us...help with issues that [the community] has been struggling with?”
The group’s collaboration with the Neighborhood Health Centers of the Lehigh Valley, which received state funding to establish a Center of Excellence for Opiate Use Disorders, grew out of those conversations. In implementing a comprehensive treatment plan, community health workers do outreach, make referrals, diagnose, prescribe a new line of opiate substitute therapy and link individuals to other needed services.
The efforts come at a critical time. In 2016, there were 4,642 fatal drug overdoses in Pennsylvania, a 37 percent increase from the previous year.
While the Neighborhood Health Centers had the funding to carry out the program, Burke says, there were no resources to assess impact. Was the program effective? He says the Lehigh group recognized the opportunity to help, given the faculty’s expertise in conducting assessments.
For her part, Lechuga is assessing the program from the provider’s perspective. She sought input from the community health workers and observed workflow. Also, she assessed protocols for recruiting patients, tracking and reporting visits, referrals and follow-up.
Burke and Napper will conduct a longitudinal study to assess the program’s implementation from the clients’ perspective. They plan to interview about 100 clients three times over a year.
Burke says it would be difficult for researchers to recruit participants on their own for a study like this one. The fact that the clients are already coming to the Center, and that the research group can talk to them too, solves a huge logistical challenge. In turn, he says, it’s crucial for the center to get needed assessment data.
Alang is exploring social integration and well-being among racially and economically marginalized populations in Allentown, Pa. She worked with the Neighborhood Health Centers, Promise Neighborhoods of the Lehigh Valley and the Lehigh Valley Health Network to collect and analyze data on the dimensions of meaningful social integration inclusion, especially within health care settings, and the connection that has to health outcomes.
As the Lehigh group continues to build relationships, Burke sees potential as a liaison between organizations and community members. “We can have our ears to the ground and listen to what the issues are from the community’s perspective and feed that back to organizations,” he says, “but also work with organizations to see what issues are on the horizon and to find ways to bring that down to community members.”
To learn more about the College of Health, go to https://www1.lehigh.edu/path-prominence
Story by: Kelly Hochbein, Mary Ellen Alu and Lori Friedman
Posted on:




